I. Introduction
The field of nursing has undergone significant changes and advancements in the 21st century. With advancements in technology, changes in healthcare systems, and evolving patient needs, nursing practice and education have adapted to meet the demands of the modern healthcare landscape. This blog post will explore the evolution of nursing in the 21st century, highlighting the changes in nursing practice and education.
Evolution of Nursing in the 21st Century
Nursing in the 21st century has seen a shift from a task-oriented approach to a more patient-centered and holistic approach. Here are some key changes and developments in the field:
1. Technology: The widespread use of technology has significantly impacted nursing practice. Electronic health records (EHRs), telehealth, and mobile applications have improved communication and accessibility of patient information, allowing nurses to provide more efficient and effective care.
2. Evidence-based Practice: The integration of research evidence into clinical decision-making has become a standard practice in nursing. Evidence-based practice ensures that nursing interventions are based on the best available evidence, improving patient outcomes and the overall quality of care.
3. Interdisciplinary Collaboration: In the 21st century, healthcare has become more team-oriented, with nurses collaborating closely with other healthcare professionals to deliver comprehensive and coordinated care. Interdisciplinary collaboration improves communication, care coordination, and patient outcomes.
Changes in Nursing Practice and Education
Nursing practice and education have also evolved to keep pace with the changing healthcare landscape. Here are a few notable changes:
1. Advanced Specializations: Nursing has expanded beyond the traditional roles of bedside care. Advanced practice nurses (APNs) now have the opportunity to specialize in areas such as nurse practitioners, nurse anesthetists, nurse educators, and nurse researchers. These advanced roles allow nurses to take on more responsibilities and contribute to improving healthcare outcomes.
2. Emphasis on Lifelong Learning: Continuous professional development and lifelong learning have become essential in nursing. Nurses are encouraged to pursue advanced degrees, certifications, and participate in ongoing education to stay updated with the latest evidence-based practices and advancements in healthcare.
3. Simulation-based Learning: Nursing education has embraced the use of simulation technology to enhance clinical competency and decision-making skills. Simulated scenarios provide a safe and controlled environment for students to practice their skills before entering real-world patient care settings.
In conclusion, nursing in the 21st century has undergone significant changes in response to the evolving healthcare landscape. These changes have focused on patient-centered care, evidence-based practice, interdisciplinary collaboration, advanced specializations, and lifelong learning. As healthcare continues to evolve, nurses will play a crucial role in providing high-quality and compassionate care to meet the needs of the diverse patient population.
II. Advancements in Technology
In the 21st century, nursing has seen significant advancements in technology that have transformed the way care is delivered. These advancements have improved efficiency, accuracy, and patient outcomes. Here are some ways technology has impacted nursing care:
Impact of Technology on Nursing Care
1. Electronic Health Records: Electronic health records (EHRs) have replaced traditional paper records, making it easier for nurses to access patient information quickly and securely. EHRs allow for seamless communication and coordination of care among healthcare providers, leading to improved patient safety and continuity of care.
2. Medical Devices: Technological advancements have led to the development of advanced medical devices that aid in patient monitoring and treatment. For example, wearable devices such as smartwatches can track vital signs and provide real-time data to nursing staff, allowing for timely interventions and proactive care.
3. Medication Administration: Technology has streamlined the medication administration process, reducing errors and improving patient safety. Automated medication dispensing systems and barcoding systems help nurses accurately administer medications and prevent medication errors.
4. Point-of-Care Testing: Point-of-care testing devices allow nurses to perform diagnostic tests such as blood glucose monitoring, cholesterol testing, and rapid strep tests at the bedside. This reduces the time it takes to obtain test results and facilitates prompt decision-making for patient care.
Telehealth and Remote Patient Monitoring
One of the most significant advancements in nursing care is the rise of telehealth and remote patient monitoring. These technologies have revolutionized healthcare delivery, especially during the COVID-19 pandemic.
Telehealth: Telehealth refers to the use of technology to provide healthcare services remotely. Nurses can conduct virtual consultations, monitor patients’ conditions, and provide education and support, all from a distance. Telehealth has improved access to care, especially for patients in rural or underserved areas, and has reduced the need for hospital visits, saving time and resources.
Remote Patient Monitoring: Remote patient monitoring involves the use of devices to collect and transmit health data from patients’ homes to healthcare providers. Nurses can remotely monitor patients’ vital signs, blood glucose levels, and other health parameters, providing proactive and personalized care. Remote patient monitoring has proven particularly useful for managing chronic conditions and reducing hospital readmissions.
These advancements in technology have not only improved the efficiency and quality of nursing care but have also enhanced patient satisfaction and outcomes. Nurses must continue to embrace and adapt to these technological advancements to provide the best possible care in the 21st century.

III. Increasing Specialization
Nursing has witnessed significant changes in the 21st century, particularly in terms of increasing specialization. As healthcare continues to evolve and become more complex, nurses have adapted to meet the diverse and specialized needs of patients. Here are some key developments in nursing specialization in the 21st century:
Emergence of Advanced Practice Nurses
One of the significant changes in nursing practice is the emergence of advanced practice nurses (APNs). APNs are highly educated and skilled healthcare professionals who provide specialized care to patients. These nurses have obtained advanced degrees, such as master’s or doctoral degrees, and possess advanced clinical knowledge and skills. APNs include nurse practitioners, clinical nurse specialists, certified nurse midwives, and certified registered nurse anesthetists.
APNs have the authority to diagnose and treat illnesses, prescribe medications, and provide primary and specialty care services. They play a crucial role in improving patient outcomes, promoting preventive care, and addressing the growing need for primary care providers. The role of APNs has not only expanded access to care but also provided more personalized and holistic care to patients.
Specialty Certification and Education
With the increasing specialization in nursing, healthcare organizations and nursing associations have recognized the need for standardized measures to assess and validate nurses’ specialized knowledge and skills. As a result, specialty certification programs have become more prevalent in the 21st century.
Nurses can pursue specialty certifications in various areas, including critical care, oncology, pediatrics, geriatrics, and mental health. These certifications require nurses to meet specific educational and experiential requirements and pass a rigorous examination. Specialty certification not only recognizes nurses’ specialized expertise but also helps ensure that patients receive the highest quality of care.
In addition to specialty certification, nursing education has also evolved to provide specialized training and preparation for nurses. Many nursing schools now offer specialized tracks or concentrations that allow nurses to focus their education and clinical experiences in specific areas of practice. This specialized education equips nurses with the knowledge and skills necessary for their chosen specialty, enabling them to provide expert care to patients.
Overall, nursing has undergone significant changes in the 21st century, with increasing specialization being one of the key developments. The emergence of advanced practice nurses and the focus on specialty certification and education have improved patient care outcomes and expanded the scope of nursing practice. These changes reflect the ever-evolving healthcare landscape and the need for highly skilled and specialized healthcare professionals.
IV. Patient-Centered Care
In the 21st century, the field of nursing has undergone significant changes, particularly in the approach to patient care. One of the key shifts in nursing practice has been towards patient-centered care, which emphasizes the importance of addressing the individual needs and preferences of patients. Here are some ways in which nursing has changed to prioritize patient-centered care:
Shift towards Holistic Care Models
- Traditionally, nursing has focused on the physical care of patients, such as administering medications and performing procedures. However, in recent years, there has been a growing recognition of the importance of addressing the emotional, social, mental, and spiritual needs of patients as well. This holistic approach to care recognizes that patients are complex individuals with unique experiences and backgrounds.
- Holistic care models often involve interdisciplinary collaboration, with nurses working closely with other healthcare professionals, such as psychologists, social workers, and chaplains, to provide comprehensive care. This collaborative approach allows for a more integrated and person-centered approach to patient care.
- Nurses now receive training in holistic care models, which includes communication and active listening skills to better understand the individual needs of patients. This enables nurses to deliver personalized care that takes into consideration the patient’s preferences, values, and beliefs.
Patient Engagement and Shared Decision Making
- Another significant shift in nursing practice is a greater emphasis on patient engagement and shared decision making. In the past, healthcare decisions were often made solely by healthcare professionals, with little input from patients. However, research has shown that involving patients in their care leads to better outcomes and increased patient satisfaction.
- Nurses now play a crucial role in facilitating patient engagement and shared decision making. They provide information and education to patients, empowering them to actively participate in their own care. This includes explaining treatment options, risks, and benefits, and helping patients make informed decisions based on their personal values and goals.
- The use of nursing informatics, such as electronic health records and patient portals, has also facilitated patient engagement. Patients can now access their health information, communicate with healthcare providers, and actively participate in their care outside of the traditional healthcare setting.
By prioritizing patient-centered care and promoting patient engagement and shared decision making, nursing in the 21st century has evolved to focus on the needs and preferences of individual patients. This shift in practice is essential for providing high-quality, personalized care that leads to better patient outcomes and experiences.
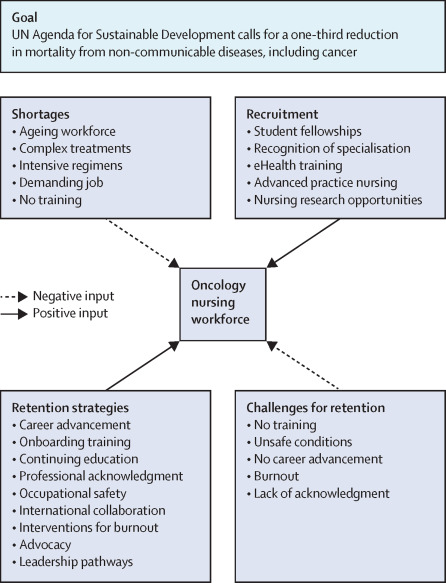
V. Nurse Shortage and Workforce Challenges
The 21st century has brought significant changes to the field of nursing, including advancements in technology, new healthcare policies, and shifting demographics. However, along with these changes, there have also been challenges that have impacted the nursing profession. One of the most significant challenges in the 21st century is the nurse shortage and workforce challenges.
Challenges in Recruitment and Retention
Recruiting and retaining qualified nurses has become increasingly difficult in the 21st century. Several factors contribute to this challenge:
1. Aging workforce: Many experienced nurses are reaching retirement age, creating a gap in the nursing workforce. This gap is challenging to fill, as new nurses need time to gain experience and develop the necessary skills.
2. Increased demand for healthcare services: The demand for healthcare services has significantly increased due to the aging population and advancements in medical technology. This increased demand puts pressure on healthcare organizations to recruit and retain enough nursing staff to meet the needs of their patients.
3. Limited resources: Many healthcare organizations face financial constraints and limited resources, making it challenging to invest in recruitment efforts and provide competitive compensation packages to attract and retain nurses.
Nurse Burnout and Strategies for Improvement
Nurse burnout has become a prevalent issue in the 21st century, resulting from the high workload, increased patient acuity, and job-related stress. Burnout not only affects nurses’ well-being but also impacts the quality of patient care.
To address nurse burnout and improve overall job satisfaction, healthcare organizations and policymakers are implementing various strategies:
1. Workload management: Healthcare organizations are working towards implementing staffing levels that align with patient needs. Adequate staffing can help reduce the burden on nurses and promote better work-life balance.
2. Supportive work environments: Creating a supportive work environment is crucial for nurse retention and satisfaction. This includes providing opportunities for professional development, fostering a culture of collaboration, and recognizing nurses’ contributions.
3. Mental health support: Recognizing the emotional toll of nursing and providing mental health support services can help nurses cope with stress and prevent burnout. This can include access to counseling services and stress management programs.
In conclusion, the 21st century has brought about significant changes in the nursing profession, but it has also presented challenges in recruitment and retention of nurses and the prevalence of nurse burnout. It is crucial for healthcare organizations and policymakers to address these challenges and implement strategies to support and retain nurses in order to meet the growing healthcare demands of the future.
VI. Diversity and Inclusion in Nursing
In the 21st century, the field of nursing has undergone significant changes, particularly in terms of diversity and inclusion. Nursing has recognized the importance of addressing cultural competence and health equity, as well as increasing diversity in the nursing workforce. These changes have been driven by a desire to provide high-quality and equitable care to a diverse patient population.
Promoting Cultural Competence and Health Equity
Cultural competence refers to the ability of healthcare professionals to effectively work with individuals from diverse cultural backgrounds. It involves understanding and respecting the beliefs, values, and practices of patients, and incorporating them into the care provided. In the 21st century, nursing has placed a greater emphasis on cultural competence to ensure that healthcare services are tailored to the unique needs of each patient. This includes:
- Providing interpreters and translators for patients who speak different languages.
- Incorporating cultural practices and beliefs into care plans.
- Recognizing the impact of socioeconomic factors on health outcomes.
By promoting cultural competence, nursing aims to reduce disparities in healthcare access and outcomes among different populations.
Increasing Diversity in the Nursing Workforce
Another important change in nursing in the 21st century has been the focus on increasing diversity in the nursing workforce. This involves recruiting and retaining nurses from underrepresented groups, such as racial and ethnic minorities, men, and individuals from lower socioeconomic backgrounds. The benefits of a diverse nursing workforce include:
- Enhanced cultural competence and ability to address the needs of diverse patient populations.
- Improved patient satisfaction and outcomes.
- Increased innovation and creativity in healthcare delivery.
To achieve greater diversity, nursing schools and healthcare organizations have implemented various initiatives, including:
- Scholarship programs for underrepresented students.
- Mentorship and support programs to help diverse students navigate the nursing profession.
- Collaborations with community organizations to promote nursing as a viable career option for diverse populations.
By increasing diversity in the nursing workforce, healthcare systems can better serve the needs of the communities they serve.
These changes in diversity and inclusion in nursing reflect a broader shift towards providing patient-centered and equitable care in the 21st century. By recognizing and addressing the unique needs of diverse patient populations, nursing professionals can contribute to improved healthcare outcomes for all.

VII. Nursing Research and Evidence-Based Practice
In the 21st century, nursing has seen significant changes, particularly in the areas of research and evidence-based practice. These advancements have greatly impacted the quality of patient care and the overall profession. Here’s a closer look at the importance of research in nursing and the integration of evidence-based practice into clinical care.
Importance of Research in Nursing
Research in nursing plays a crucial role in advancing the field and improving patient outcomes. Some key reasons why research is important in nursing include:
1. Improving Patient Care: Research helps nurses identify the most effective interventions and treatments, leading to improved patient outcomes. It provides evidence-based guidelines that healthcare professionals can follow to optimize care.
2. Advancing Nursing Knowledge: Research expands the body of nursing knowledge and contributes to ongoing professional development. It helps nurses stay up-to-date with the latest practices and techniques, allowing them to provide the highest standard of care.
3. Enhancing Patient Safety: Research helps identify potential risks and pitfalls in healthcare settings. By studying patient safety practices and implementing evidence-based interventions, nurses can help minimize errors and improve the safety of patient care.
Integration of Evidence-Based Practice into Clinical Care
Evidence-based practice (EBP) is an approach that combines the best available research evidence with clinical expertise and patient preferences. It emphasizes the use of evidence-based guidelines and protocols to guide clinical decision-making. Here are some key aspects of integrating evidence-based practice into clinical care:
1. Guiding Clinical Decision-making: Evidence-based practice provides healthcare professionals with up-to-date and reliable information to inform their clinical decisions. It helps nurses utilize research findings to guide their practice and make informed choices about patient care.
2. Promoting Quality and Safety: By integrating evidence-based practice into clinical care, nurses can ensure that the care they provide is based on the latest research and best practices. This promotes quality and safety in patient care and minimizes variations in practice.
3. Continual Learning and Improvement: Evidence-based practice encourages nurses to continually update their knowledge and skills. It fosters a culture of lifelong learning and improvement, ensuring that nurses stay current with the latest research and advancements in the field.
Overall, the integration of research and evidence-based practice in nursing is essential for improving patient outcomes, advancing the profession, and ensuring the delivery of high-quality and safe care. By staying informed about the latest research and implementing evidence-based guidelines, nurses can make a significant impact on the health and well-being of their patients.
VIII. Conclusion
Impact of 21st Century Nursing Changes
In the 21st century, nursing has undergone significant changes that have had a profound impact on the profession. The advancements in technology, the shifting demographics of patients, and the evolving healthcare landscape have all contributed to these changes. Some key impacts of 21st century nursing changes include:
- Increased Technological Integration: The rapid advancement of technology has revolutionized nursing practice. Electronic medical records, telehealth, and remote monitoring systems have improved patient care, enhanced communication among healthcare teams, and increased efficiency in delivering nursing services.
- Focus on Preventive Care: With a growing emphasis on preventive care, nurses are increasingly involved in educating patients about healthy lifestyles and disease prevention. The role of nurses as primary care providers has expanded, with a focus on managing chronic conditions and promoting wellness.
- Interdisciplinary Collaboration: In response to the complex healthcare needs of patients, interdisciplinary collaboration has become essential. Nurses now work closely with physicians, pharmacists, social workers, and other healthcare professionals to provide comprehensive care. This collaboration improves patient outcomes and promotes a more holistic approach to healthcare.
- Increased Demand for Specialized Nurses: As healthcare becomes more specialized, there is a growing demand for nurses with specialized knowledge and skills. Advanced practice nurses, such as nurse practitioners and nurse anesthetists, are playing an increasingly important role in healthcare delivery, particularly in underserved areas.
Future Directions for the Nursing Profession
Looking ahead, there are several key areas in which the nursing profession is expected to evolve:
- Embracing Artificial Intelligence and Big Data: As technology continues to advance, nurses will need to adapt to the use of artificial intelligence and big data in healthcare. This includes utilizing predictive analytics to identify at-risk patients, optimizing treatment plans, and improving patient outcomes.
- Addressing Health Disparities: Nurses have a unique opportunity to address health disparities by providing culturally sensitive care, advocating for underserved populations, and promoting health equity.
- Leadership and Policy Advocacy: Nurses are increasingly taking on leadership roles in healthcare organizations and shaping healthcare policy. Their expertise and insights are invaluable in influencing the delivery of quality care and improving patient outcomes.
- Lifelong Learning and Professional Development: The rapidly evolving nature of healthcare demands that nurses engage in lifelong learning and continuous professional development. Keeping up with new research, technologies, and best practices is crucial for providing high-quality care.
In conclusion, nursing in the 21st century has been transformed by technological advancements, changing patient demographics, and the evolving healthcare landscape. These changes have had a significant impact on the profession, from increased technological integration to a focus on preventive care. As the nursing profession continues to evolve, nurses will need to embrace new technologies, address health disparities, take on leadership roles, and prioritize lifelong learning and professional development. By doing so, they will continue to be at the forefront of providing quality care and making a positive impact on patient outcomes.
Thank you for taking the time to read our latest blog post on EliteCare.net We hope you found the information valuable and insightful. Your health and well-being are our top priorities, and we strive to provide you with the best advice and resources.






